
Preliminary Observations from Emergency and Critical Care
Written by Martrin Gutierrez, RN, BSN, SRNA, DNAP (student)
And Yisel Menendez RN, BSN, SRNA, DNAP (student)
A Preliminary Observational Survey on Peripheral Venous Access in Real Clinical Environments
Peripheral intravenous access remains one of the most frequently performed procedures in modern medicine. However, despite its frequency, clinicians who perform this procedure daily report that obtaining venous access can become significantly difficult in certain patients and clinical contexts.
In order to better understand how this procedure is experienced in real clinical practice, a preliminary observational survey was conducted among 36 healthcare professionals actively involved in vascular access procedures.
The purpose of this initiative was not to evaluate a specific device or test a technological intervention, but rather to document perceptions and experiences from frontline clinicians who routinely perform this procedure.
Participants and Clinical Context
Participants included professionals with varying levels of experience, ranging from clinicians with only a few years of practice to operators with more than 15–20 years of experience in high-intensity hospital environments.
Most participants work in high-pressure clinical settings, particularly emergency departments and intensive care units.
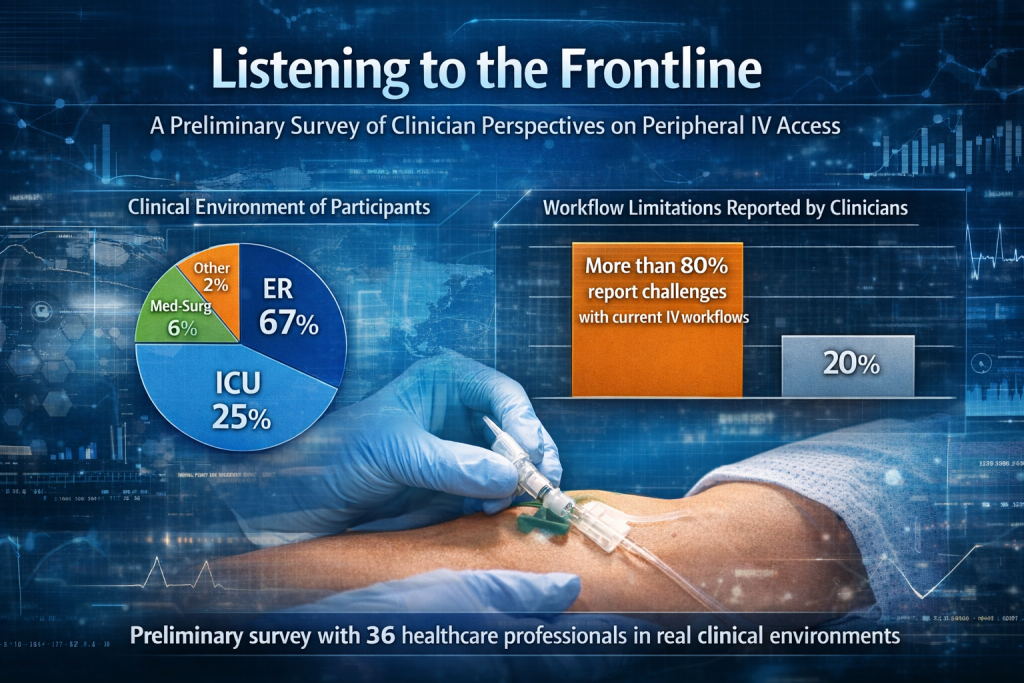
Figure 1. Clinical environment of participants (n=36)
Emergency Department — 24
ICU — 9
Med-Surg — 2
Other clinical environments — 3
These data indicate that the vast majority of collected opinions come from professionals who perform vascular access in environments where speed and procedural efficiency are critical.
Figure 2. Participants in high-pressure clinical environments
ER + ICU — 33 participants
Other environments — 3 participants
In other words, more than 90% of participants work in areas where venous access must often be obtained rapidly and repeatedly during a clinical shift.
Observations from Clinical Practice
Across different levels of experience and clinical contexts, participants described peripheral venous access as a procedure that is often straightforward in patients with visible or palpable veins, but considerably more complex in patients with difficult intravenous access (DIVA).
Clinicians frequently mentioned factors that complicate the procedure, including:
- obesity
- dehydration
- chronic disease
- repeated hospitalizations
- poorly visible or palpable veins
- emergency situations where access must be obtained under extreme pressure, such as patients arriving via EMS in cardiac arrest, severe trauma, or active hemorrhage, where the movement of the resuscitation environment, limited space, and the urgent need to administer critical medications can further complicate vein localization
In these situations, multiple insertion attempts are not unusual, particularly in emergency settings, combat environments, or critical care units.
These observations reflect structured impressions from professionals who routinely perform this procedure in clinical practice.
Perceived Limitations in Clinical Workflow
In addition to discussing procedural difficulty in certain patients, many participants also identified limitations related to the integration of technological tools into the clinical workflow.
In the survey conducted, 30 of the 36 participating clinicians (83%) indicated that having tools that improve operator autonomy or reduce the need to wait for additional equipment could significantly improve the vascular access process.
This observation is particularly relevant in emergency settings, where time, mobility, and immediate access to resources can directly influence patient care.
Several works in the clinical literature, such as Ultrasound-Guided Peripheral Intravenous Catheter Insertion: The Nurse’s Manual published in Critical Care Nurse (2020)
https://doi.org/10.4037/ccn2020240
note that ultrasound-guided IV placement “has not been as rapidly adopted in the critical and acute care nursing realms.”
This supports our argument that although technologies such as ultrasound can improve vascular access in certain situations, their adoption within everyday clinical workflow remains limited outside specialized teams.
The opinions collected in this preliminary survey reflect a similar perception among frontline clinicians.
The Importance of Listening to Frontline Clinicians
Medical innovation often begins with a deep understanding of how procedures are actually performed in daily practice.
By gathering perspectives from professionals who perform vascular access in real clinical environments, this preliminary survey seeks to contribute to a better understanding of the challenges that persist in one of the most common procedures in medicine.
Although these observations represent an initial exploratory effort, they highlight the importance of incorporating frontline clinical experience when analyzing widely practiced medical procedures.
Conclusion
Peripheral intravenous access remains one of the most frequently performed procedures in healthcare. However, even among experienced clinicians, situations persist in which obtaining vascular access becomes complex.
This preliminary survey involving 36 healthcare professionals provides an initial look at how clinicians perceive these challenges in real working environments.
The collected observations suggest that although the procedure is routine, operational difficulties remain and opportunities exist to improve the integration of technological tools within the clinical workflow.
Understanding these perspectives may help guide future research on the evolution of vascular access in clinical practice.
Written by Martrin Gutierrez, RN, BSN, SRNA, DNAP (student)
And Yisel Menendez RN, BSN, SRNA, DNAP (student)mpatibility, and real-world clinical needs.
